Table of Contents
Renal Fascia Overview
The renal fascia (perirenal fascia) is a capsule or covering of the kidney. it was originally defined as having two distinct layers. The posterior layer was known as the Zuckerkandall fascia and the anterior layer was the Gerota fascia.
Laterally, these two fasciae fused to form the lateral conal fascia. The lateral conal fascia continues anterolaterally behind the colon to merge with the parietal peritoneum.
Read Renal Plasma Flow
Recent Anatomical Studies of Renal Fascia
However, recent research has shown that the fascia is made up of a single multi-laminated structure that is fused posteromedially with muscular fasciae of the psoas major and quadratus lumborum muscles.
The fascia then extends anteromedially behind the kidney as a bi-laminated sheet, which divides at a variable point into a thin layer that runs around the front of the kidney as the anterior perirenal fascia and a thicker posterior layer that runs anterolaterally as the lateral conal fascia.
It was previously thought that the anterior and posterior perirenal fasciae fused above the suprarenal gland and then fused to the diaphragmatic fascia, but research now shows that the superior part of the perirenal space is “open” and in continuity with the bare region(bare area) of liver on the right side and with subphrenic extraperitoneal space on the left side.
The anterior fascia merges with the inferior coronary layer and the bare region of the liver on the right side at the level of the upper pole of the kidney.
The anterior layer fuses with the gastrophrenic ligament on the left side.
The posterior layer fuses with fasciae of muscles of the posterior abdominal wall, such as the psoas major and quadratus lumborum, as well as fascia on the inferior part of the thoracoabdominal diaphragm on both the right and left sides.
The anterior layer is continuous from one kidney to the other, and the posterior layer is connected to either side of the vertebra.
Both layers stretch along the ureter and merge with the iliac fascia below.
Read Renal Blood Flow
Importance and Function of Renal Fascia
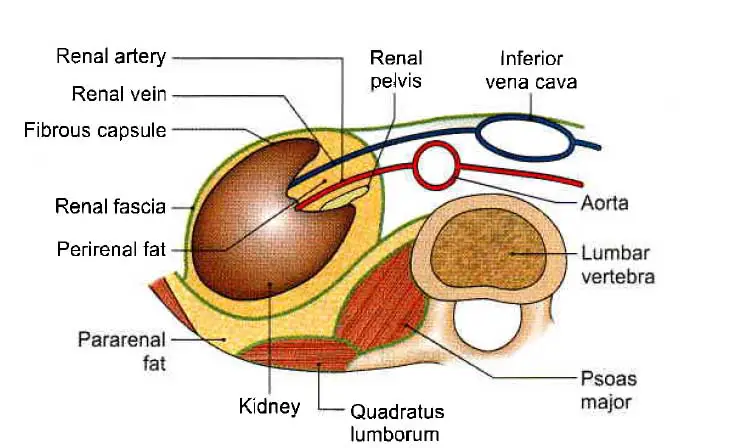
The renal fascia is a capsule or covering of the kidney that separates the perirenal fat from the pararenal fat. It can be seen on a radiograph and aids in the accurate localization of abdominal masses. It is also helpful in separating perinephric hematomas and abscesses from intrarenal or subcapsular hematomas and abscesses.
Read Renal Infarction
Clinical Anatomy of Renal Fascia
- Blood from a ruptured kidney or pus from a perinephric abscess first distends the renal fascia before forcing its way downward through the pelvis. Because of the fascial septum and the midline attachment of the renal fascia, it cannot cross to the opposite side.
- Inside the renal fascia, a floating kidney may travel up and down but not side to side.
- In this case, the posterior layer of the renal fascia can be sutured with the diaphragm and the kidney can be kept in place.
Read Renal Parenchymal Disease
Capsule or covering of the kidney
The Fibrous Capsule
This is a thin membrane that wraps around the kidney and lines the renal sinus. Normally, it is quickly removed from the kidney, but in some disorders, it becomes adherent and cannot be removed.
Perirenal or Perinephric Fat
This is an adipose tissue layer that exists outside of the fibrous capsule. It is thickest at the kidney’s margins and fills the extra space in the renal sinus.
Renal Fascia
Read the above discussions
Pararenal or Paranephric Body (Fat)
It is made up of a variable amount of fat that lies outside the renal fascia. It is more abundant in the kidney’s posterior and lower poles. It forms a cushion for the kidney by filling the paravertebral gutter.
Exposure of kidney from behind
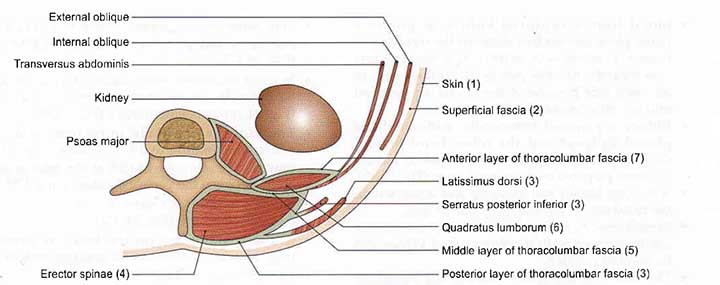
The following layers must be reflected one by one when revealing the kidney from behind.
- Skin
- Superficial fascia
- Posterior layer of thoracolumbar fascia with latissimus dorsi and serratus posterior inferior
- Erector spinae, which can be removed for convenience
- The middle layer of the thoracolumbar fascia
- Quadratus lumborum
- The anterior layer of thoracolumbar fascia in which the related nerves are embedded.
Dissection of the Kidney
Remove the fat and fascia from the anterior surface of the left and right kidneys, as well as the suprarenal glands. Trace the left suprarenal vein then the left testicular or ovarian vein to get to the left renal vein. Follow this vein from the left kidney to the inferior vena cava, noting any tributaries along the way. Displace the vein to reveal the left renal artery, then follow its branches to the left suprarenal gland and ureter. In the abdomen, follow the ureter.
Determine the structures associated with the anterior surface of both kidneys. Turn the left kidney medially to reveal its posterior surface, and take note of the relationship between its vessels and the ureter. Determine the muscles, arteries, and nerves posterior to the kidneys.
Repeat the dissection on the right side. The right testicular or ovarian veins, as well as the suprarenal veins, drain directly into the inferior vena cava.
Cut across the kidney’s convex boundary before you reach the hilus. Take a look inside. Recognize the cortex, pyramids, and calyces.
Follow the ureters through the renal pelvis, the abdomen, the pelvic cavity, and eventually through the urinary bladder wall.
Read Disodium Hydrogen Citrate
Location of the kidney
The kidneys are located in the epigastric, hypochondriac, lumbar, and umbilical regions of the body. They are placed vertically from the upper border of the twelfth thoracic vertebra to the center of the body of the third lumbar vertebra. The right kidney is lower than the left, and the left kidney is closer to the median plane than the right.
The transpyloric plane runs through the upper part of the right kidney’s hilus and the lower part of the left kidney’s hilus.
Few Last Words
Renal Fascia is anatomically important to know before exploring dissection and renal studies. As well as renal fascia is clinically important as we discussed before it helps to localize the abdominal masses and helps to separate the abscess and masses.
Last Updated on February 23, 2022 by Learn From Doctor Team






