Table of Contents
Renal Infarction
Renal Infarction is or acute renal infarction that starts with mild flank pain and subsequently fever, nausea, and vomiting. High blood pressure(Hypertension) and oliguria can be present. Renal infarction should be treated as an emergency because it can lead to complete kidney failure.
Differential diagnosis of renal infarction
Renal infarction can be mistaken with;
- Nephrolithiasis: The condition nephrolithiasis (kidney stones) affects the urinary tract. Kidney stones are small deposits of calcium, phosphate, and other food components that form in the kidneys. They are one of the most common causes of blood in the urine(Hematuria).
- Pyelonephritis: Acute pyelonephritis is a serious kidney infection that occurs suddenly. It causes the kidneys to swell and damage them permanently.Chronic pyelonephritis is a disease that occurs when attacks are repetitive or recurrent. The chronic type is uncommon, but it affects children and people with urinary obstructions more frequently.
Pyelonephritis is a life-threatening condition.
Clinical features of kidney Infarction
- Severe epigastric pain(radiating toward the back)
- Watery stool with blood
- Intense vomiting(It is the main cause that people come to the hospital to admit)
- Pain similar to Cholecystitis
- High blood pressure
- Irregular heartbeat
- Diffuse abdominal tenderness
- Positive hemoccult test
- Malena

Sign and symptoms may include;
- Fever
- Nausea
- Diarrhea
- Flank pain
- Sometimes oliguria
Read Renal Parenchymal Disease
Diagnostic Criteria of renal infarction
Physical examination
- Hypertension
- Arrhythmia
- Diffuse abdominal tenderness
- Ill looking
- Weakness

On laboratory investigations
There aren’t any ideal laboratory investigation criteria for renal infarction, lab investigations results match with kidney stone results;
Here is a laboratory analysis of a renal infarction patient(case study):
| Test | Result | Normal Value |
| White blood cells | 28.9 | 4.8–10.8 × 109/L |
| Neutrophils | 27.5 | 2.0–7.5 × 109/L |
| Lymphocytes | 0.6 | 1.5–4.0 × 109/L |
| Monocytes | 0.8 | 0.11–1.0 × 109/L |
| Eosinophils | 0.0 | (0.0–0.35 × 109/L |
| Basophils | 0.0 | 0–0.2 × 109/L |
| Red blood cells | 5.07 | 4.2–5.4 × 1012/L |
| Hemoglobin | 137 | 120–160 G/L |
| Platelets | 300 | 130–400 × 109/L |
| Serum sodium | 141 | 135–145 mmol/L |
| Serum potassium | 4.4 | 3.5–5 mmol/L |
| Blood urea nitrogen | 7.9 | 3–7 mmol/L |
| Serum creatinine | 52 | 37–91 μmol/L |
| Serum amylase | 365 | 20–160 U/L |
| Serum lactate dehydrogenase | 485 | 115–220 U/L |
Other investigations analysis
The abdominal x-rays can reveal a gas distribution that is not specific. There may no mention of a fluid level. Cardiomegaly with calcification and unfolding of the thoracic aorta can be seen on a chest x-ray. There may no signs of pancreatitis or stones on an abdominal CT scan. The left kidney may have a large or small focal area of infarction and the right kidney had a small or large focal area of infarction, indicating significant atherosclerosis of the superior mesenteric artery. There may no sign of ischemic bowel or perforation. There can be a few diverticuli here and there, but no signs of diverticulitis. At the base of the left lung, there can be evidence of air space disease.
Radiological Diagnosis
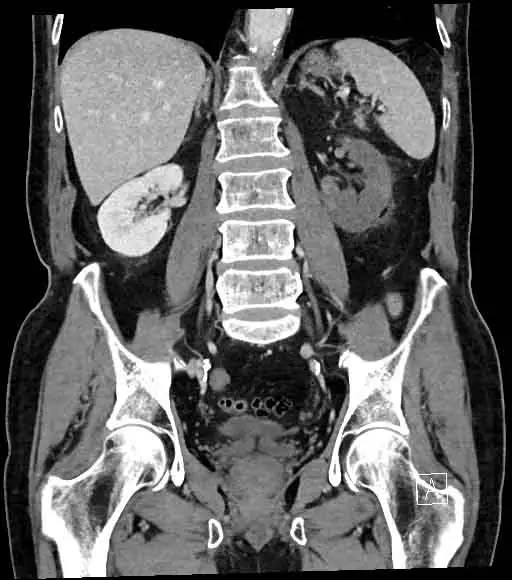
CT Scan
The occluded vessel can be seen on a CT angiogram. In the event of a trauma, it’s crucial to check for a hematoma at the hilum, which may signify transection. The renal vein can also be occluded in rare cases.
Post-contrast images, ideally in the cortical/arterial phase, are the best way to spot renal infarcts. There are one or more focal, wedge-shaped parenchymal defects that spread to the capsular surface and affect both the cortex and the medulla. When the main renal artery is blocked, the entire organ fails to function properly.
Ultrasound
Although CT is normally the first course of action, ultrasound can be used if the clinical picture is unclear.
Acute infarction will appear as a lack of perfusion on a color Doppler test in such cases. If the whole kidney is affected, there may be no perfusion, or it could be patchy if segmental arteries are involved. The lack of flow can also be seen in the renal artery and, in rare cases of venous thrombosis resulting in infarction, the renal vein.
Infarction wounds shrink over time, becoming hyperechoic scars.
Risk factors of renal infarction
- Atrial fibrillation
- previous history of infarction
- Pulmonary embolism
- Valvular or Ischemic heart disease
Read Renal Blood Flow
Treatment of renal infarction
During the first week of renal infarction, many patients experience elevated blood pressure, which normally reduces unless the patient has underlying hypertension. Antihypertensive drugs, especially angiotensin-converting enzyme inhibitors or angiotensin receptor antagonists, may be helpful.
Since there are no comparative studies, the best approach for renal infarction caused by thromboembolism, in situ thrombosis, or renal artery dissection is unknown. Anticoagulation, endovascular therapy (thrombolysis/thrombectomy with or without angioplasty), and open surgery have all been mentioned.
In this situation, the normal anticoagulation regimen is intravenous heparin supplemented by oral warfarin. Depending on the cause of renal infarction, the target INR can change. The typical goal is 2.0–3.0. If incidents recur despite sufficient INR or in high-risk patients, such as those with rheumatic heart disease or a prosthetic valve, a higher target of 2.5–3.5 is appropriate.
Thrombolysis, thrombectomy, or angioplasty with or without stenting are both examples of percutaneous endovascular therapy. Local intra-arterial injection of a thrombolytic agent reduces the risk of bleeding when on thrombolytic therapy. 9 Only patients with atrophic kidneys or a history of prolonged ischemia should be treated for reperfusion therapy. Renal infarction is treated with anticoagulation in the majority of patients with thromboembolic disease, although certain patients have a specific sign, such as atrial fibrillation. There are no studies that compare anticoagulation, local thrombolytic treatment, or catheter thrombectomy to surgery. The majority of the evidence is outdated, with studies from 1970 to 1982 claiming an 11 percent operative mortality rate.
Few last words
Renal infarction is a condition that is frequently overlooked due to its vague appearance. In an individual with atrial fibrillation, sudden onset of severe abdominal pain with nausea and vomiting, as well as elevated aspartate transaminase and lactate dehydrogenase, there should be a strong suspicion of renal infarction.
The key to a quick recovery is early diagnosis and anticoagulation.
Last Updated on February 23, 2022 by Learn From Doctor Team






