Table of Contents
Overview
Renal Parenchymal Disease also known as Kidney Parenchymal disease, Bilateral Renal Parenchymal Disease, and Renal Parenchyma of Kidney.
To learn about the renal parenchymal disease first, we have to know the basic anatomy of the kidney.
Basic Anatomy of the Kidney
The parenchyma is a functional part of a kidney that filters blood and makes urine. Structurally the parenchyma is divided into two areas;
- An outer reddish-brown cortex: Nearly one million nephrons in the renal cortex (which have glomeruli, Bowman’s capsule which are the primary filterers of blood flowing through the kidney, and renal tubules, which adjust the amount of fluid by reabsorption and secretion to create the perfect amount/content of urine) are found in the renal cortex.
- An inner pale medulla: The medulla’s principal purpose is to control urine concentration. The urine flows from the collection tubes into the renal calyces and pelvis and is drained into the downstream ureter and bladder by a single directional peristaltic motion.
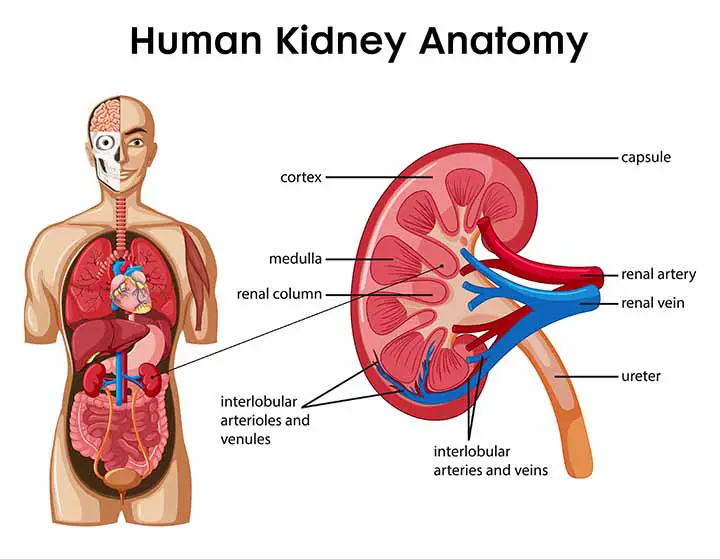
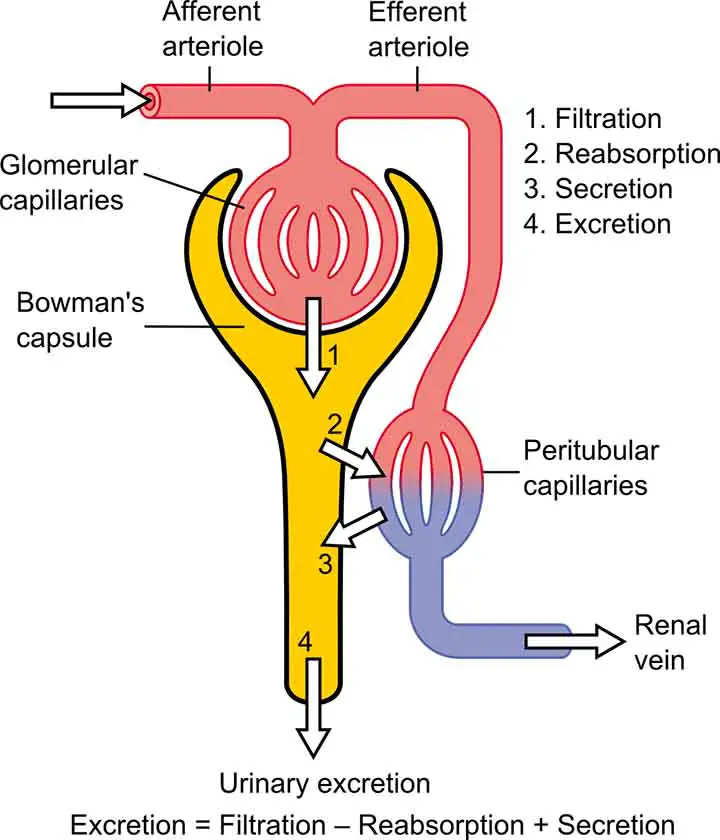
Renal parenchymal disease means the disease or medical conditions that damage the above-mentioned parts of the kidney. Those conditions can be congenital, acquired, or associated with other diseases and conditions.
Read Renal Blood Flow
Renal Parenchymal Disease Causes
- Congenital disease and conditions such as; polycystic kidney disease, Multicystic dysplastic kidney, etc.
- Genetic conditions are passed from the parents by chromosomes.
- Infections(viral or bacterial)
- Stones in the kidney
- Hypertension
- Diabetes mellitus
- Certain autoimmune diseases such as; nephritis with purpura etc.
- Certain medication or drug effects.
Read Renal Infarction.
Renal Parenchymal Disease Symptoms
Most people are aware that one of the kidneys’ primary functions is to remove wastes and extra water from the body. The urine removes these waste products as well as excess liquid.
Urine is made up of a series of highly complex excretion and re-absorption steps. This process is needed to maintain a chemically stable equilibrium in the body.
The kidneys are in charge of controlling the body’s sodium, potassium, and acid levels. Hormones produced by the kidneys have an impact on the function of other organs. A hormone released by the kidneys, for example, stimulates the development of red blood cells.
Other hormones released by the kidneys aid in blood pressure regulation and calcium metabolism regulation.
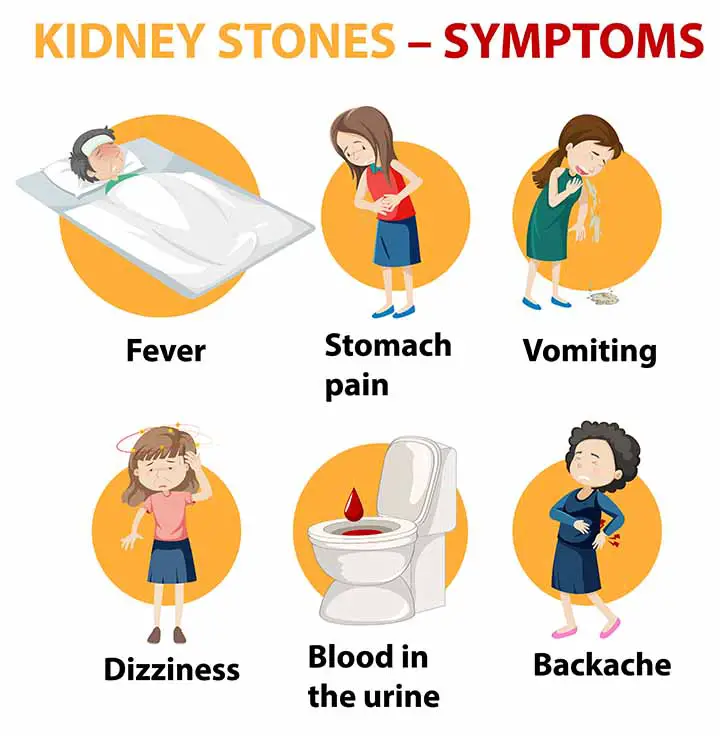
The kidney parenchymal disease hampers the functioning of the kidney and arises signs and symptoms;
- Edema (hand, feet, body)
- Hypertension(sometimes severe)
- Anemia
- Bone changes(due to deficiency of calcium)
- Hematuria(blood passes through urine)
- Abdominal swelling
Renal Parenchymal Disease Signs
- Loss of appetite
- Itching all over the body
- Nausea
- Vomiting
- Fatigue and weakness
- Joint pain
- Dizziness
- Frequent night urination
Renal Parenchymal Disease Diagnosis
Blood Tests
A blood test is the most common test for any kidney disease. The test checks the amount of creatinine, a waste product, in your blood.
Your doctor calculates how much waste your kidneys should be able to filters in a minute based on your blood test results, as well as your age, height, gender, other medical conditions, and ethnic group.
eGFR is the approximate glomerular filtration rate that is the result of this blood test.
Kidneys in good health should be able to filter more than 90 milliliters per minute. If your renal filtration rate is lower than this, you might have the renal parenchymal disease.
Urine Test
A urine test is performed to:
- The albumin: creatinine ratio, or ACR, is a measurement of the levels of albumin and creatinine in your urine.
- Inspect your urine for blood or protein.
Urine checks, in addition to your eGFR, will help you get a clearer understanding of how well your kidneys are functioning.
Imaging Test
The doctor may recommend you to do an ultrasound of the kidney structures.
Other Tests
Other tests can be used to determine the severity of your kidney damage or disease.
- An ultrasound scan, MRI scan, or CT scan can be used to examine the kidneys to decide if any blockages occur.
- A kidney biopsy involves removing a small sample of kidney tissue with a needle and examining the cells under a microscope for signs of damage or irritation.
Renal Test Results Interpretation
Your test results will help you figure out how badly your kidneys are affected.
This will aid your doctor in determining the best course of action for you as well as how you can have tests to track your condition.
eGFR results can be categorized into five stages:
- Stage 1 (G1): a normal eGFR above 90ml/min along with other indications of renal parenchymal damage.
- Stage 2 (G2): a slightly diminished eGFR of 60 to 89ml/min along with other indications of renal parenchymal damage.
- Stage 3 (G3): an eGFR of 30 to 59ml/min, stage 3 can be divided into 3a(g3a) 45-59 ml/min and 3b(g3b) 30-44 ml/min.
- Stage 4 (G4): an eGFR of 15 to 29ml/min.
- Step 5 (G5): an eGFR of less than 15ml/min, indicating that the kidneys have almost completely lost their function.
ACR results can be categorized into 3 stages:
- A1: an ACR of less than 3mg/mmol
- A2: an ACR of 3 to 30mg/mmol
- A3: an ACR of more than 30mg/mmol
Both eGFR and ACR indicate the severity of kidney damages. The higher the stage is the more severe the condition is. These tests help the doctor to determine the renal parenchymal disease and the severity of the conditions.
Renal Parenchymal Disease Treatment
It depends on the severity of the condition. Firstly doctors try to manage the disease and conditions with some medication, then fluid management, low metabolites, and salt intake, dialysis, and in some complicated cases, you may have to replace your kidney.
Treating the Cause
Your doctor will try to delay or stop the progression of your kidney disease by treating the underlying cause. Depending on the cause, there are a variety of treatment options. Even an underlying condition such as hypertension can worsen kidney conditions and need to be controlled.
Treating The Complications
- Hypertension medications: High blood pressure can worsen in people who have kidney disease or conditions. Your doctor may prescribe medications to lower your blood pressure and maintain kidney function, such as angiotensin-converting enzyme (ACE) inhibitors or angiotensin II receptor blockers. Since high blood pressure drugs may reduce kidney function and alter electrolyte levels at first, you can need regular blood tests to keep track of your progress. A diuretic (water pill) and a low-salt diet are likely to be prescribed by your doctor.
- Medication prescribed to lower the cholesterol level: To lower your cholesterol, your doctor may prescribe statin medications. High levels of bad cholesterol are common in people with kidney parenchymal disease, which can raise the risk of cardiovascular disease.
- Anemia medications: In certain cases, the doctor may prescribe erythropoietin supplements, which may include iron. Erythropoietin supplements promote the production of more red blood cells, which may help to alleviate anemia-related tiredness.
- Oedema medications: Fluid retention is a risk for patients with the renal parenchymal disease. Swelling in the legs, as well as high blood pressure, may result. Diuretics are medications that help keep the body’s fluid balance in check.
- Medication to keep the bones healthy: To prevent weak bones and reduce your chances of fracture, your doctor recommends calcium and vitamin D supplements. A phosphate binder is a form of medication that lowers the amount of phosphate in your bloodstream and protects your blood vessels from calcium deposits (calcification).
- A lower protein diet: Your body produces waste products when it absorbs protein from food, which your kidneys must remove from your blood. Your doctor may advise you to eat less protein to make work easier for your kidneys have to do. Your doctor can also refer you to a dietitian who will advise you about how to reduce your protein intake while maintaining a balanced diet.
Treatment for the severe renal parenchymal disease
In the end stage of renal parenchymal disease, the kidneys cannot excrete the amount of wastage produced by the body and you develop a near-complete or complete renal failure.
The treatment at this stage is following;
Dialysis
When your kidneys are no longer able to do so, dialysis is used to extract waste products and excess fluid from your blood. A system removes waste and excess fluids from your blood during hemodialysis.
A thin tube (catheter) inserted into your abdomen fills your abdominal cavity with a dialysis solution that collects waste and excess fluids during peritoneal dialysis. The dialysis solution removes from the body after an amount of time, taking the waste with it.
Kidney Transplantation
A kidney transplant is when a healthy kidney from a donor is surgically implanted into your body. Kidneys may be transplanted from either dead or living donors. To prevent the body from rejecting the new organ, you’ll need to take drugs for the rest of your life. A kidney transplant does not require you to be on dialysis.
Takeaway
The renal parenchymal disease can be minor and severe. Minor conditions can be treated with medication and diet. But if the situation is severe then you need dialysis or kidney transplantation.
The third choice for those who do not want dialysis or a kidney transplant despite having a severe renal parenchymal disease is to treat kidney failure with conservative steps. When you have total kidney failure, though, your life expectancy is normally just a few months.
Last Updated on April 13, 2022 by Learn From Doctor Team






