Table of Contents
Stercoral Colitis Overview
Stercoral Colitis is a quite rare inflammatory condition that occurs when the fecal material causes the distension of the colon and leads to fecaloma formation.
That fecaloma can consequence focal pressure necrosis and eventually perforation. On the other hand, colonic distension and pressure can lead to diminished vascular supply and eventually ischemic colitis.
There are multiple points in the colon that are prone to ulceration. Among them the most common are the;
- Sigmoid Colon
- Rectum
The risk factor for stercoral colitis is chronic constipation. There are some other risk factors as well, such as dementia, prolong bed lying patients, young patients with some specific psychiatric conditions.
Among the risk factors, the most common one is constipation, more specifically chronic constipation.
Causes of The Stercoral Colitis
Stercoral colitis doesn’t appear suddenly. It undergoes some steps or processes. It occurs when chronic constipation causes or leads to fecal impaction, colonic deformation, and distension. The accumulation of dehydrated fecal material is known as fecalomas.
The fecaloma accumulates in some specific areas of the colon, usually the sigmoid colon or rectum. This causes ischemic pressure ulceration in that area and that leads to ischemic focal necrosis and perforation.
According to some studies around 27% of patients develop colonic ulceration in multiple areas. This condition leads to multiple complications such as; edema, ischemia, etc. We will discuss these complications later in this article.
The specific causes for stercoral colitis are multifactorial, these include;
- Chronic constipation
- Low fiber diet
- Not drinking enough water
- Genetical factors
- Behavioral patterns
- Medication side effects
- Physiological and pathological conditions
All the factors that cause constipation, affect colonic motility and absorption cause stercoral colitis.
Read Erythematous Mucosa of the Antrum|Gastritis
Risk Factors of Stercoral Colitis
- People with chronic constipation
- Prolonged bed lying patients
- Chronic opioid users
- Young patients with psychological conditions
- Improper diet
- Eating less dietary fibers
- Not eating enough water
- People who don’t involve in any physical activity.
- Elder peoples who are taking many medications
Parents should not be relieved that children cannot be affected by stercoral colitis. If they did not train about toiled hygiene, eating habits, and hygienic lifestyle, children can be affected too.
Pathophysiology of Stercoral Colitis
Fecaloma occurs when the dehydrated fecal matter accumulates in the colonic area due to chronic constipation. The stagnation of a high volume of fecal matter causes deformation of the colon.
Hardened fecal material aka fecaloma accumulates in certain areas of the colon, usually the rectosigmoid region. The fecaloma compressed the wall of the colon and related vasculature. It interprets the blood supply and when the blood supply cannot meet the cellular demand it leads to ulceration, ischemia, and necrosis.
Ulceration arises in the region adjacent to the fecaloma, generally in the antimesenteric side of the bowel. This is because the blood supply arises from the mesentery. As the antimesenteric part of the bowel is affected, the ischemia is also more likely to affect this side of the bowel.
This ischemia can lead to necrosis and perforation, if not treated at the appropriate time, this can be life-threatening.
According to some research, 77% of the stercoral colitis/ulceration occurs in the sigmoid colon or rectum. The reason behind it is, when the fecal material reaches the rectosigmoid area it eventually becomes dehydrated while reaching there. Also, it is the narrowest area in the colon.
Usually, the lodged fecal material or fecaloma does not compress the whole area. On rare occasions, the obstructed bowel compresses the entire vasculature of equal to its size. Which can lead to diffuse compression of the veins and interfere with the outward flow of blood. Eventually, this leads to intramural edema, arterial compromise, and ischemic colitis.
If the colon involvement is more than 40% and also there is perforation, this can be extremely life-threatening.
Diagnosis of Stercoral Colitis
Physical Examination
On physical examination patient usually shows diffuse abdominal tenderness on palpation and abdominal distension. On digital rectal examination, stool can be found in the rectal vault as well as a small volume of stool can be passed out, this DRE helps to differentiate between stercoral colitis and intestinal obstruction.
When the case is severe, there can be peritonitis, septic shock, or multiorgan failure, if the colonic ischemia and perforation have already occurred.
Medical History
The history of chronic constipation is present in almost every case of stercoral colitis. Causes of constipation can include different metabolic, psychiatric, or neurologic conditions. Elderly patients with chronic constipation are at high risk of stercoral colitis. If the patient is in bed lying for any health condition for a longer period, this can also be a risk factor.
The symptom of stercoral colitis are common, these are; abdominal pain, discomfort, and fever.
Investigations
Although, the laboratory investigations for stercoral colitis are nonspecific, still, some blood tests are necessary to prevent sepsis and septic shock in severe cases. Leukocytosis and acute phase reactants evaluation is also done in most cases.
- Blood Culture
- Blood screening
- Blood Coagulation test
- Blood Typing
As the lab tests are non-specific, imaging tests are mandatory for the diagnosis of stercoral colitis. If the patient is suspected of perforation and has peritonitis, there should be an upright chest x-ray for confirmatory diagnosis.
The ultimate key for diagnosis is CT abdomen and pelvis with IV contrast. Make sure if the patient’s renal function is normal or not.
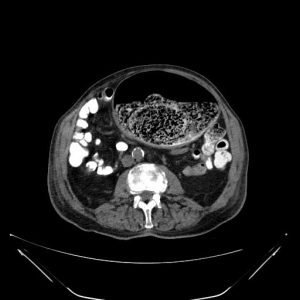
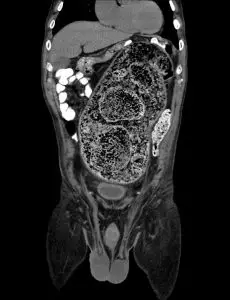
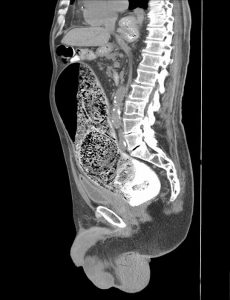
Findings of CT in Stercoral Colitis
- Fecal impaction with dilation of the colon, generally the rectosigmoid colon
- The entire colon can show fecal impaction if the patient presents late
- In some cases, fecaloma can be present as radiopaque masses within the colon
- If edema and ulceration present in a case secondary to pressure necrosis, there will be focal thickening of the wall adjacent to the fecaloma. This will appear as a mucosal discontinuity in CT Imaging.
Mucosal Discontinuity is marked by a decreased update of IV contrast in some areas of the bowel wall where blood supply is diminished. This evaluation refers to stercoral colitis from uncomplicated fecal impaction, usually where the colonic wall is thin.
- Pericolonic fat stranding also can be evaluated from CT. Which refers to stercoral colitis.
If there are extraluminal bubbles or abscess is present that indicates perforation has already occurred. Intraoperative and histologic studies are necessary to diagnosis if surgery is required or not.
Differential Diagnosis
- Diverticulitis
- Intestinal obstruction
- Large bowel obstruction
- Ulcerative colitis
- Infectious colitis
- Malignancy
- Bowel perforation
- Acute mesenteric ischemia
- Intra-abdominal abscess
Treatment of Stercoral Colitis
If the patients don’t show any signs of peritonitis, can be treated non surgically by manual disimpaction via the rectum. The alternatives of this procedure include;
- Endoscopically guided disimpaction
- Bowel regimen
The patient should be admitted for close monitoring before and after the disimpaction.
It’s not sure that surgical management is required or not, patients should be kept NPO for safety purposes. Opioids medication should not be used to treat pain because they reduce colonic motility. If the patients show signs of sepsis or septic shock, they should be resuscitated as needed with intravenous fluids and broad-spectrum IV antibiotics, that cover gram-negative as well as anaerobic organisms.
Patients with perforation need surgical management.
If a large section of the bowel is involved in any patient or the conservative treatment fails, the treatment procedure for these patients requires;
- Resection of the affected bowel
- Colostomy
- Hartmann pouch
The management of Stercoral Colitis is not done until you treat chronic constipation. The treatment of chronic constipation includes;
- Increase the intake of dietary fiber in the diet
- Proper medication for preventing future constipation
- Health and diet education for patients to understanding how constipation occurs.
- Osmotic and stimulant laxatives can be considered as the first-line treatment of constipation.
Read Drinking a gallon of water a day
Prognosis
The prognosis depends on some factors. The diagnosis, present condition, previous medical history.
The highest rate of mortality is in perforation, which is about 32-59%. Other than that the mortality occurs if a large segment of the bowel is affected (more than 40cm), and in ischemic bowel, that shows symptoms such as; elevated lactic acid or septic shock. There is no proper evidence for age or sex difference for mortality.
Though the mortality is caused mainly by perforation, the main culprit is stercoral colitis.
Possible Complications
As we already mentioned that the most serious complication is perforation. The mortality rate for this is as high as 32-59%. Other complications include; septic shock and ischemic colitis. Urinary retention can occur due to compression of the dilated bowel.
- Multiorgan failure may occur as a result of sepsis and hypoperfusion.
- Renal failure can occur as a result of compression and obstruction of ureters.
- Patients who were treated non surgically can experience recurrence of ulceration because of the perforation of the colon in the segment which was affected.
- Patients who were treated surgically can come up with leakage of anastomosis and resulting sepsis.
Stercoral Colitis Summary
Sterocoral colitis is quite a rare inflammatory colitis that is caused by fecal impaction. That may lead to perforation, ischemic necrosis, ulcer formation, and colonic perforation by increasing the colonic intraluminal pressure.
This can be treated both surgically and non surgically according to the condition. The major consequence of stercoral colitis is perforation, which accounts for 32-59% of mortality.
The main cause behind stercoral colitis is chronic constipation. there can be some other causes too, such as psychological problems, prolonged bed lying coma patients.
Last Updated on February 15, 2022 by Learn From Doctor Team






